Why Your Face Ages the Way It Does
Introduction: Ageing Has an Anatomy
If you have looked in the mirror and wondered why your face looks tired when you are not, or why lines appear in specific places rather than uniformly, the answer lies beneath the surface — in the layered anatomy of the face itself.
“The pathogenesis of facial aging may be explained on an anatomical basis. An anatomical approach to surgical rejuvenation of the face provides the way to obtaining a ‘natural’ result that is lasting and with minimal morbidity.”
This is the foundational principle behind modern facial surgery — and it is what separates treatments that look natural from those that look operated. Understanding facial anatomy is not just a surgical concern. For patients considering any form of facial rejuvenation, it is the essential framework for making informed decisions.
The Five Layers of the Face
The soft tissues of the face are arranged in five concentric layers. “The five concentric layers of the face are: (1) skin; (2) subcutaneous tissue; (3) musculoaponeurotic layer; (4) loose areola tissue; (5) deep fascia.”
This five-layered arrangement is most clearly seen in the scalp and forehead, where the underlying cranial vault has expanded to accommodate the human frontal lobe — creating a generous, easy-to-study version of the same layered structure that exists throughout the face. In the cheek and lower face, the same five layers exist but are more compacted and complex, due to the reduced forward projection of the mid and lower face and the dominance of the orbital and oral cavities.
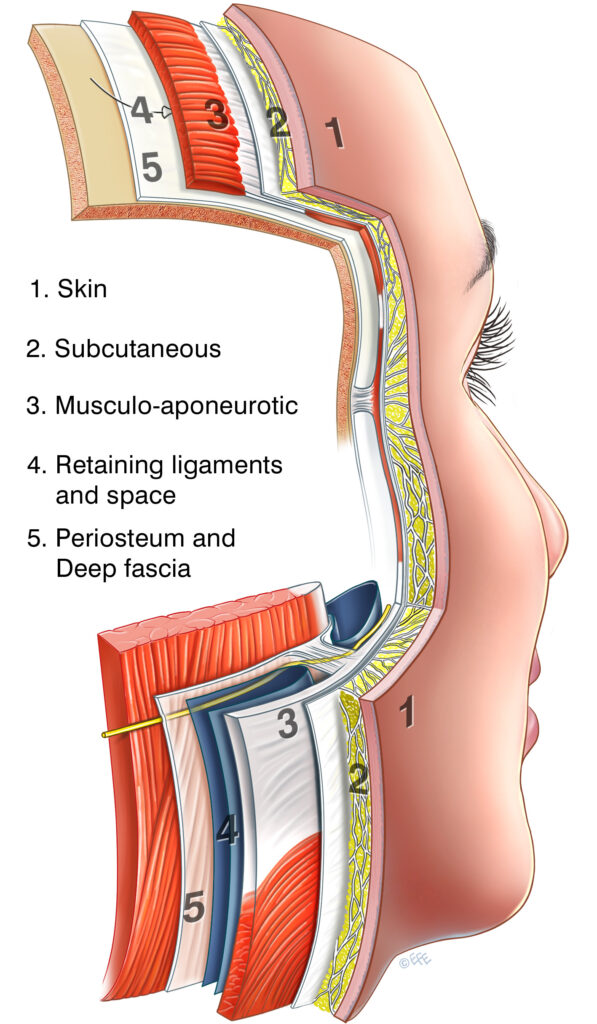
What this diagram shows: A cross-section of the scalp and face illustrating all five layers stacked concentrically. The scalp shows the clean prototype — galea (layer 3), subgaleal space (layer 4), and periosteum (layer 5) — while the facial section shows the same five layers with the complexity introduced by the orbital and oral cavities, the alternating spaces and ligaments in layer 4, and the transition paths of the facial nerve branches.
Layer 1 — Skin
The epidermis is rich in keratinocytes, with melanocytes and Langerhans cells also present. Beneath it, the dermis contains a rich vascular plexus and provides structural integrity. “The thickness of the dermis relates to its function and tends to be inversely proportionate to its mobility. The dermis is thinnest in the eyelids and thickest over the forehead and the nasal tip. The thinner the dermis, the more susceptible it is to qualitative deterioration ageing changes.”
Skin ageing is driven by genetics, UV exposure, hormonal changes, and metabolic processes. With age, “the supple skin of youth becomes thinned and flattened, with loss of elasticity and architectural regularity.” At a molecular level, the number of fibroblasts decreases, as do collagen levels — particularly types I and III — and elastin. Both chronological ageing and photoageing promote matrix metalloproteinase (MMP) expression, which degrades collagen, while simultaneously reducing procollagen synthesis.
Oxidative stress — the accumulation of reactive oxygen species (ROS) — is considered of primary importance in driving this process. Smoking accelerates it dramatically: “Other environmental factors, notably smoking, accelerate skin ageing by between 10 and 20 years.” The mechanisms include increased collagenase activity and decreased skin circulation.
The muscles of facial expression compound the picture. “As the underlying collagen weakens and the skin thins, the dermis loses its capacity to resist the constant force of the muscles and these lines become etched in the skin, ultimately even at rest.”
Layer 2 — Subcutaneous Tissue
The subcutaneous layer has two components: subcutaneous fat (which provides volume) and the **retinacular cutis** — the fibrous tissue that binds the dermis to the underlying SMAS. “The retinacular cutis is the name given to that portion of the retaining ligament that passes through the subcutaneous tissues.”
The structure of the retinacular cutis is architecturally elegant: it resembles a tree, with “fewer but thicker fibres deep as it rises through the SMAS that progressively divide into multiple fine microligaments as they reach the dermis.” This explains why subcutaneous dissection is easiest at the deeper level (just above the SMAS surface) — there are fewer fibres there. Conversely, dissection close to the dermis is tighter and requires more precision.
The retinacular cutis fibres are not uniform across the face. Over retaining ligaments, they are dense and vertically oriented. Over the soft tissue spaces between ligaments, they are sparser and horizontally oriented — which is why tissue over the spaces can be separated with simple blunt dissection while tissue over the ligaments requires sharp release.
The subcutaneous fat itself is not a uniform layer. It is compartmentalised into discrete units by the retaining ligaments, which form their boundaries. Named compartments — the malar fat pad, the nasolabial fat — reflect the prominence of fat in specific anatomical zones. In youth, the transitions between compartments are smooth and invisible. “With ageing, a series of concavities and convexities develop which separate these compartments.”
Importantly, current evidence indicates that “fat descends minimally with ageing. Distinct compartmentalization by the retaining ligaments holds the fat in its relative position.” What changes is not the position of the fat, but the visibility of the ligamentous boundaries between compartments — as those boundaries weaken and the intervening spaces enlarge.
Layer 3 — The Musculoaponeurotic Layer (SMAS)
“The muscles of facial expression are unique and fundamentally different from skeletal muscles beneath the deep fascia because they are situated within the superficial fascia and they move the soft tissues of which they are a part.”
This is what makes the face extraordinary. Unlike muscles elsewhere in the body — which contract to move bones relative to each other — the facial muscles contract to move the skin itself. They live within the superficial fascia (layers 1–3) and are directly bonded to the overlying dermis, so their contraction immediately moves the skin surface.
This entire muscular layer is called the **Superficial Musculoaponeurotic System (SMAS)**. It is “continuous over the entire face, although for descriptive purposes, different names are given to certain parts according to the superficial muscle within.” Over the scalp it is the galea aponeurotica; over the temple it is the temporoparietal fascia; around the eye socket it is the orbicularis fascia; over the mid and lower face it is the SMAS proper; and in the neck it is the platysma.
Within layer 3, the muscles are arranged in two sub-layers. The broad, flat superficial muscles — frontalis (upper face), orbicularis oculi (midface), platysma (lower face) — have minimal direct bony attachment and are stabilised at their periphery by the retaining ligaments. The deeper muscles provide functional control of the eyelid and lip sphincters, including the zygomaticus major and minor, levator labii superioris, and the depressor muscles around the mouth.
With ageing, the mimetic muscles of the face behave differently from skeletal muscles. Skeletal muscles can atrophy by up to 50% with age. The face’s mimetic muscles — in constant use with expression — appear more resistant. Research confirms the orbicularis oculi remains histologically unchanged, with no loss of muscle fibres or ptosis with ageing. However, “the upper lip orbicularis atrophies with ageing, with decreased muscle thickness, smaller muscle fascicles, and increase in surrounding epimysium.”
Layer 4 — The Space and Ligament Layer
This is the most complex and surgically significant layer. It is the plane in which sub-SMAS facelift surgery is performed, and it contains four key structures:
1. Soft tissue spaces
2. Retaining ligaments
3. Deep parts of the intrinsic muscles (passing from their bone attachment to their superficial soft tissue origin)
4. Facial nerve branches, transitioning from deep to superficial
“Functionally, a series of soft tissue spaces exist in layer 4 to allow independent movement of the periorbital and perioral muscle of facial expressions (located in the roof of the facial soft tissue spaces) over the deep fascia on the major muscles for mastication directly beneath (located beneath the floor of the facial soft tissue spaces).”
The retaining ligaments are strategically placed at the boundaries between these spaces. In the lateral face — directly in front of the ear — there is a diffuse area of ligamentous attachment called the **platysma auricular fascia (PAF)**, where the dermis, subcutaneous tissue, SMAS, and underlying parotid capsule are all bound together. Layer 4 here is reduced to a fused layer, with no soft tissue space present.
Layer 5 — Deep Fascia and Bone
“The deep fascia, the deepest soft tissue layer of the face is formed by the periosteum where it overlies bone.” Over the lateral face, where the temporalis and masseter muscles of mastication cover the bone, the deep fascia is instead the deep temporal fascia and masseteric fascia respectively. The parotid fascia is also part of layer 5, as is the deep cervical fascia in the neck.
“The deep fascia, although thin, is tough and unyielding and gives attachment to the retaining ligaments of the face.”
The Retaining Ligaments: The Face’s Suspension System
The retaining ligaments are the structural backbone of facial architecture — and the anatomical basis of every visible groove on the ageing face.
“To secure the mobile superficial layers to the facial skeleton, an elaborate system of retaining ligaments bind the dermis to the skeleton (or deep fascia where the facial skeleton is covered by skeletal muscles for mastication); the components of this system pass through all layers.”
Their structure can be visualised as a tree: “The ‘trunk’ of the ligaments attach the soft tissues to the periosteum of the facial skeleton or deep muscle fascia. The ligaments pass through all soft tissue layers, fanning out as multiple branches through the SMAS to eventually insert into the dermis. The ligamentous component in the subcutaneous layer is seen as the retinacular cutis.”
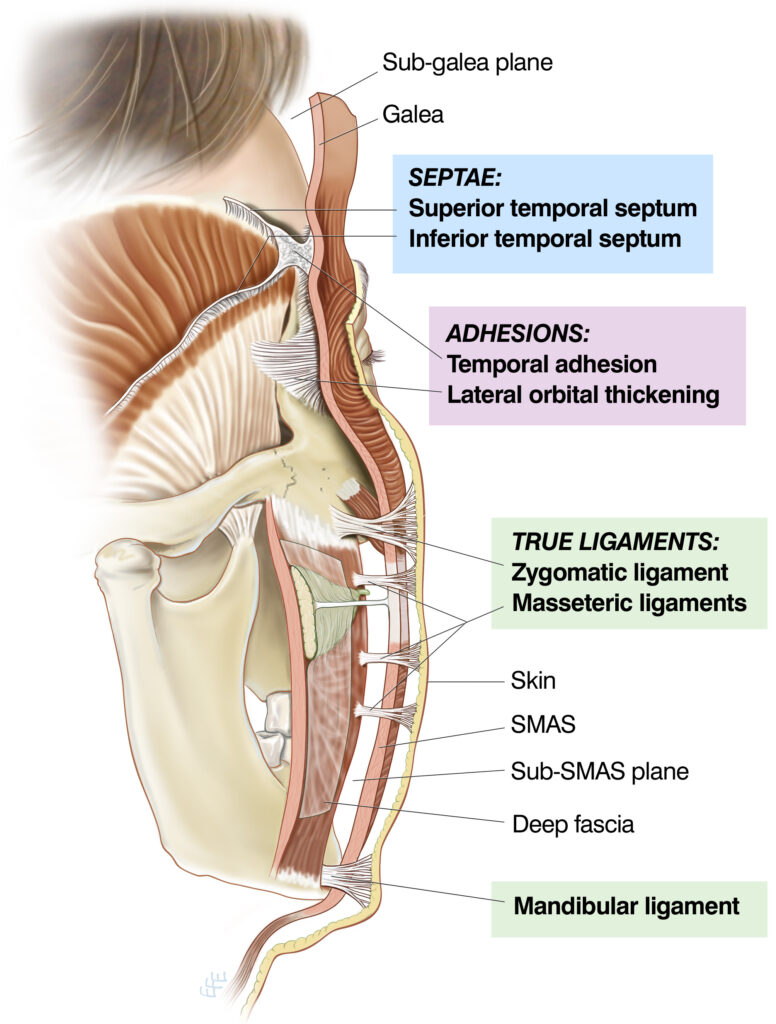
What this diagram shows: A schematic cross-section of the facial layers with the ligament drawn as a tree whose trunk anchors to the periosteum (layer 5), whose main branches pass through the SMAS (layer 3), and whose multiple fine terminal branches (retinacular cutis) insert into the dermis (layer 1). The retaining ligaments appear in three morphological forms across the face: A lateral cross-section of the face illustrating the three forms the retaining ligaments take — septae (wall-like sheets, such as the superior and inferior temporal septa), adhesions (broad zones of ligamentous fusion, such as the temporal adhesion and lateral orbital thickening), and true ligaments (discrete, named osteocutaneous anchors: the zygomatic ligament, masseteric ligaments, and mandibular ligament). The skin surface, SMAS, sub-SMAS plane, and deep fascia are all labelled, showing where each ligament type exists in the layered system. True osteocutaneous ligaments** anchor directly from bone to dermis — the zygomatic ligament, mandibular ligament, and tear trough ligament are the most clinically significant. Septa are wall-like structures (the superior and inferior temporal septa). Adhesions are diffuse zones of ligamentous fusion (the temporal adhesion, the lateral orbital thickening, the platysma auricular fascia).
The visible grooves on the ageing face — tear troughs, palpebromalar grooves, nasolabial folds, jowl lines — correspond precisely to where these ligaments attach to the skin surface. The skin is tethered inward at the ligament; the adjacent tissue sags forward; the result is the characteristic groove-and-bulge pattern of ageing.
The Facial Soft Tissue Spaces: Where Ageing Originates
Between the retaining ligaments in layer 4 are the soft tissue spaces. These spaces are anatomically significant for two reasons: they are the areas where age-related laxity originates, and they are the safest planes for surgical dissection.
“These spaces have defined boundaries that are strategically reinforced by retaining ligaments. Significantly, from a surgical perspective, these areas are by definition anatomically ‘safe spaces’ to dissect, as no structures cross within and all branches of the facial nerve are outside these spaces.”
“As the roof of each space is the least supported part, laxity is more prone to develop here with ageing, compared to their ligament-reinforced boundaries. This differential laxity accounts for much of the characteristic changes that occur with aging.”
What this diagram shows: 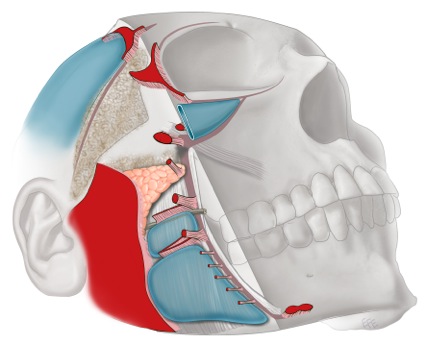 A lateral view of the skull and soft tissue, colour-coded to show the anatomical organisation of layer 4. Blue zones represent the soft tissue spaces (upper temporal, prezygomatic, premaxillary, premasseter). Red zones represent retaining ligaments. Stippled triangular areas just above and below the zygomatic arch mark the locations where the temporal and zygomatic branches of the facial nerve pass from deep to superficial — the most critical zones for surgical awareness. The platysma auricular fascia (PAF) is shown as the large area of ligamentous fusion covering the parotid region.
A lateral view of the skull and soft tissue, colour-coded to show the anatomical organisation of layer 4. Blue zones represent the soft tissue spaces (upper temporal, prezygomatic, premaxillary, premasseter). Red zones represent retaining ligaments. Stippled triangular areas just above and below the zygomatic arch mark the locations where the temporal and zygomatic branches of the facial nerve pass from deep to superficial — the most critical zones for surgical awareness. The platysma auricular fascia (PAF) is shown as the large area of ligamentous fusion covering the parotid region.
The Key Facial Spaces
Upper Temporal Space
Above the temple, two compartments are separated by the obliquely oriented inferior temporal septum. The upper compartment is a true anatomical space — safe for blunt dissection. The lower triangular compartment contains critical anatomy: the temporal branches of the facial nerve run “parallel to and immediately inferior to this septum” on the underside of the temporoparietal fascia. The sentinel vein, visible during surgical dissection, is not a reliable landmark for the temporal nerve — the nerve travels cephalad to the vein, between it and the inferior temporal septum.
Prezygomatic Space
This triangular space overlies the body of the zygoma, with the orbicularis oculi in its roof and the origins of the zygomatic muscles beneath its floor. Its function is to allow the orbicularis to contract independently of the zygomatic muscles. With ageing laxity, the roof sags. “This aging of the prezygomatic space, with bulging over its roof accentuated by its well-supported boundaries, is the anatomical basis for the clinical entity variously described as malar mounds, bags or malar crescent.”
Premaxillary Space
This quadrangular space overlies the maxilla, medial to the prezygomatic space. “This space is clinically significant in that laxity over its roof contributes to the deepening of the nasolabial fold with ageing.” It also provides a safe sub-SMAS plane for surgical correction of the tear trough deformity.
What this diagram shows: A frontal/oblique view of the midface showing the premaxillary space in its anatomical context. The key neighbouring structures — the infraorbital nerve, the tear trough ligament, the orbicularis retaining ligament, and the levator labii superioris — are all labelled, illustrating why this space is surgically important for both nasolabial fold correction and tear trough treatment.
Lower and Middle Premasseter Spaces
These spaces overly the masseter muscle, allowing jaw movement without distorting the overlying skin. The lower premasseter space has the platysma as its roof. Its clinical significance is profound: it is the direct anatomical basis of jowl formation. “Laxity in the roof of the space, particularly where it has a weakened attachment to the anterior masseter by the masseteric ligaments and its inferior boundary where there is no ligament, manifests as the labiomandibular fold and jowl respectively.”
**What this diagram shows:** A lateral dissection of the lower face illustrating the rhomboidal premasseter space. The platysma roof, the PAF posterior boundary, and the weak inferior mesenteric-like boundary are all shown. The mandibular branch of the facial nerve is traced running under the inferior boundary of the space and rising to the mandibular ligament — its course explaining both its vulnerability and its variability. The buccal fat pad and buccal space are shown anterior to the space.
—
The Facial Nerve: Why Anatomy Determines Safety
The facial nerve is the most critical structure in facelift surgery — and understanding its relationship to the layered anatomy is what allows safe, deep-plane surgery.
“The danger zones for facial nerve injury have been well described in the literature, but this is of limited value to the surgeon due to the topographical 2-dimensional perspective this gives of the expected course of the nerve relative to surface landmarks. Confidence when approaching the nerve surgically comes from (1) an understanding of the 3-dimensional course of the nerve relative to the layered anatomy as described above and by (2) visually identifying the nerves in relation to defined landmarks.”
The facial nerve branches exit the parotid gland and remain deep to layer 5 in the lateral face. As they approach the anterior face, they traverse layer 4, ascending to reach the underside of the mimetic muscles. “It is at these transition points across layer 4 that the nerves are at greatest risk of injury. The transitions occur at predictable locations, in close association with retaining ligaments that, being immobile, provide stability and protection for the nerves.”
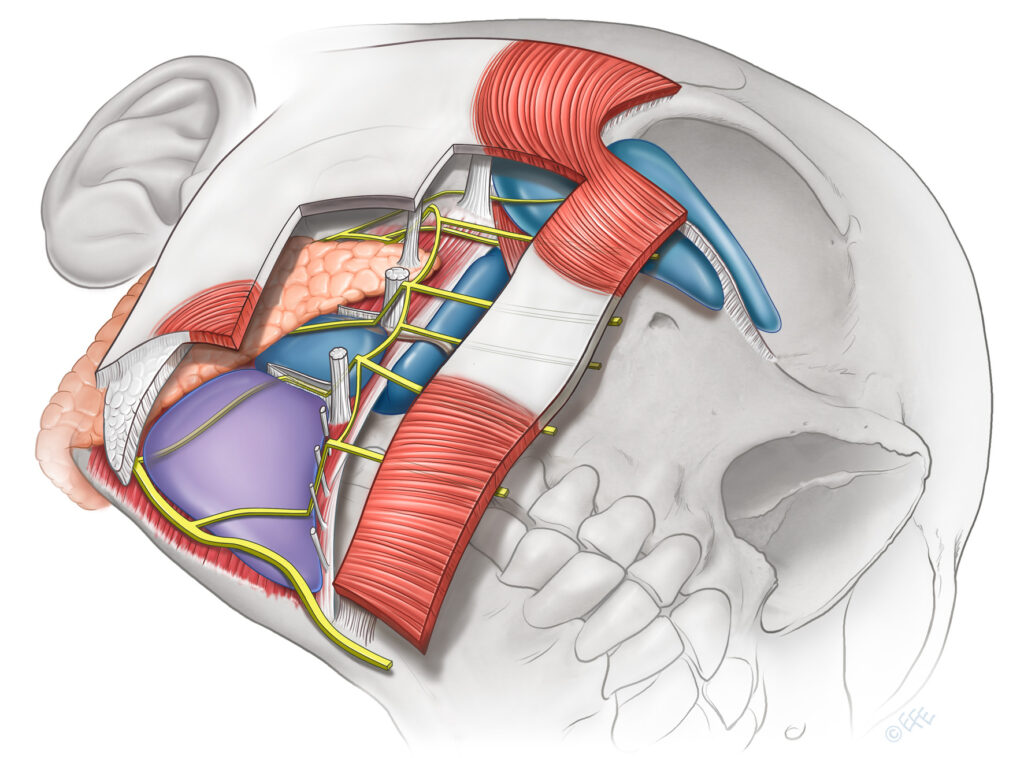
What this diagram shows: A composite illustration of the lateral face showing all major facial nerve branches — temporal, zygomatic, upper and lower buccal, and mandibular — in their correct anatomical positions relative to the soft tissue spaces and retaining ligaments. The nerves are shown running deep to the spaces in the lateral face, then transitioning through layer 4 to layer 3 at the ligamentous boundaries. The interconnecting branches between nerve trunks — which provide the anatomical basis for functional recovery after partial nerve injury — are also shown.
The temporal branch runs along the Pitanguy line (from 0.5 cm below the tragus to 1.5 cm lateral to the supraorbital rim). It was traditionally believed to run just deep to the SMAS as it crosses the zygomatic arch — making high SMAS incisions dangerous. Histological research has since shown “that the temporal branches are in transition from where they exit the parotid below the zygomatic arch, to where they enter the underside of the temporoparietal fascia some 2 cm above the arch” — running in layer 4, protected by the parotid-temporal fascia all the way through. This understanding has validated the high SMAS technique.
The temporal and mandibular branches are the most surgically significant because their target muscles lack cross-innervation. The marginal mandibular branch is at risk at two points — near the angle of the mandible (within the PAF) and anteriorly near the mandibular ligament. Between these fixed points, the nerve is mobile, travelling within the inferior membranous boundary of the premasseter space.
How Each Region of the Face Ages
Temple and Forehead
The frontalis muscle raises the brow and forehead skin, but “anatomically, the frontalis muscle ends at approximately the temporal fusion line (superior temporal septum). Lateral to this, there is not an upward vector to counteract the downward pull of the medial and lateral brow depressors and gravity on the lateral brow, which may explain why more descent occurs at the lateral brow.”
The medial brow, in contrast, seldom descends with ageing and may actually rise — because the frontalis compensates for the downward pull of the corrugator and procerus by maintaining chronic hypertonicity.
The skin over the temple is thinner and less firmly supported than the forehead, reflecting the large underlying temporal space and the nature of the temporal septa — which, unlike other facial ligaments, do not continue into the subcutaneous layer to fix the dermis.
The Midcheek: Three Segments, Three Grooves
“A smooth rounded midcheek is a powerful image of youth. With aging, the three midcheek segments become clearly discernible, as they become separated by the three cutaneous grooves of the midcheek: the nasojugal, palpebromalar, and midcheek grooves. This ‘segmentation’ of the midcheek has a profound impact on appearance that is responsible for giving the ‘tired’ look associated with aging.”
The three segments each overlie a specific part of the facial skeleton:
– The **lid-cheek segment** overlies the inferior orbital rim
– The **malar segment** overlies the body of the zygoma
– The **nasolabial segment** overlies the anterior surface of the maxilla
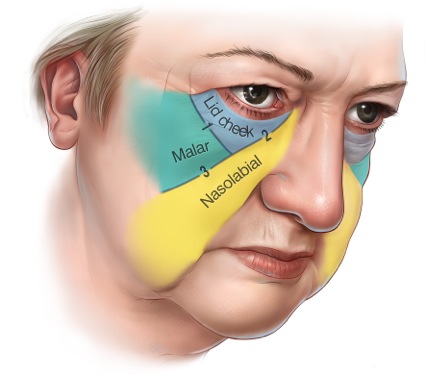
What this diagram shows: A three-quarter view of an ageing face with the three midcheek segments colour-coded (blue, green, yellow) and the three grooves between them (palpebromalar, nasojugal, and midcheek groove) traced. The Y-shaped pattern of the grooves is clearly visible, and the correspondence between each segment and its underlying skeletal region is shown. This diagram makes immediately intuitive why midcheek ageing creates the “tired” appearance — the seamless midcheek of youth fragments into three distinct, groove-separated units.
The Tear Trough
“The tear trough ligament is a true osteocutaneous ligament originating from the maxilla and inserting into the dermis of the tear trough, passing through and binding all five soft tissue layers together.” It is the direct anatomical cause of the tear trough deformity.
Laterally, the tear trough ligament continues as the **orbicularis retaining ligament (ORL), which is the anatomical basis for the palpebromalar groove. “The continuity of the tear trough ligament with the orbicularis retaining ligament then explains the observation that with more advanced aging, the tear trough becomes continuous with the palpebromalar groove, forming the prominent cutaneous groove sometimes called a prominent ‘lid–cheek junction.'”
The Lower Face: Jowls and Labiomandibular Fold
The jowl and labiomandibular fold do not exist in youth — they are purely products of ageing. Their mechanism is now fully understood.
“With the onset of aging, laxity develops in the roof of the premasseter space associated with attenuation of the anterior and inferior boundaries. The major retaining ligaments (the key masseteric and mandibular) in contrast remain relatively strong and at these locations the superficial fascia remains firmly fixed to the underlying deep fascia.”
Distension of the weaker masseteric ligaments at the anterior border of the lower premasseter space allows the buccal fat to descend — this is the anatomical basis of the labiomandibular fold. The mandibular ligament then demarcates the transition from labiomandibular fold above to jowl below. “The jowl develops as a result of distension of the roof of the lower premasseter space with resultant descent of the tissues below the body of the mandible. The more prominent the jowl, the more apparent will be the cutaneous tethering provided by the mandibular ligament.”
The Role of Bone Loss
“The facial skeleton changes dramatically with aging and this has a profound impact on the appearance of the face with aging.”
After reaching peak skeletal projection in early adulthood, selective areas of the facial skeleton undergo significant resorption. The most affected areas are the midface (maxilla, including the pyriform area of the nose), the superomedial and inferolateral aspects of the orbital rim, and the prejowl area of the mandible.
What this diagram shows: A three-quarter view of the skull with arrows marking each zone of age-related bone resorption. Arrow size indicates the relative magnitude of loss at each site. The midface (maxilla and pyriform area) and the superomedial and inferolateral orbital rim are the most heavily marked, with additional resorption shown at the prejowl mandible. This diagram makes visible the invisible — the skeletal changes that underlie so much of what we observe on the surface.

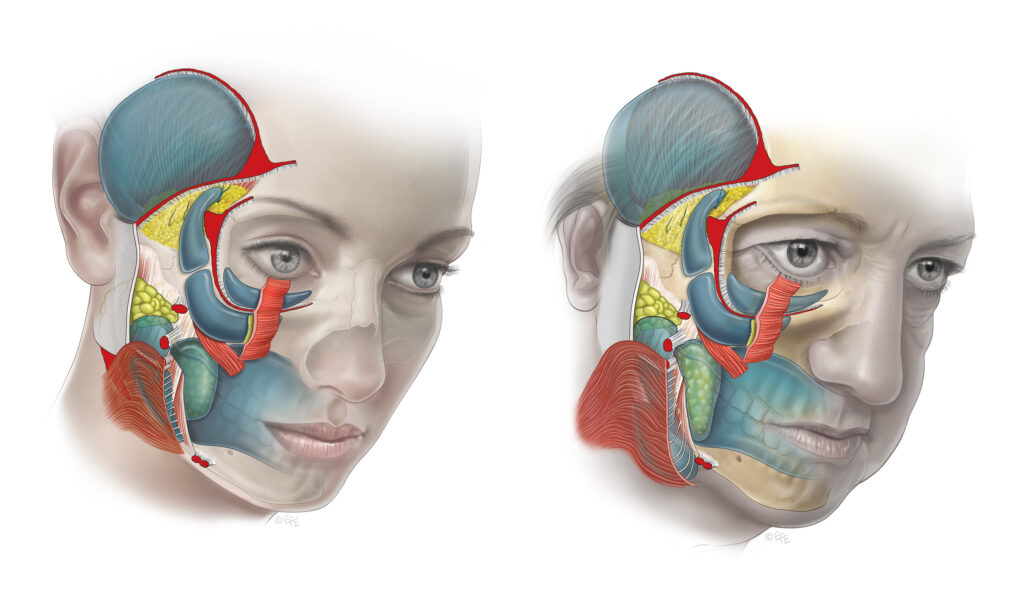
What this diagram shows: A paired image — skull on the left with stippling marking areas of bone loss, aged face on the right — placed side by side to demonstrate the precise spatial correspondence between skeletal resorption and surface ageing signs. Midface retrusion corresponds to tear trough deepening and nasolabial fold prominence. Orbital rim resorption corresponds to the lengthened lower eyelid appearance. Prejowl mandible resorption corresponds to the jowl-mandible interface. This is one of the most powerful images in the textbook for communicating why volume restoration and structural support are essential components of facial rejuvenation.
“Retrusion of the facial skeleton causes the origin of the multilinked fibrous retaining ligaments to be displaced posteriorly. This pulls the skin inwards, exaggerating the concavity between the areas of relative convexity that develop with aging. Retrusion of the midcheek with loss of projection gives the visual impression of tissue descent with aging.”
Importantly, “some patients have a congenitally weak, meaning inadequately projecting, skeletal structure. In such cases, the skeleton may be the primary cause of the manifestations of premature aging. Accordingly, in patients who suffer premature facial aging, a weakness of the relevant part of the underlying skeleton is immediately suspect and should be addressed in order to obtain better esthetic results.”
How Ageing Evolves Across the Face’s Spaces and Ligaments
“The multilinked fibrous system attenuates with aging, with decreasing strength of the ligaments and increasing laxity. In general, the spaces expand with aging in proportion to the amount of movement. This is greatest with the lower premasseter space and the related mandibular movement, and least over the zygoma.”
In young people, the spaces are more potential than real and do not open easily. With ageing, “the spaces dissect easily in older patients, and the boundaries widen as the ligaments weaken” — a surgical observation with direct clinical relevance.
Why Anatomy-Based Surgery Works
Understanding facial anatomy transforms surgical planning from empirical guesswork into logical, predictable correction.
“Once a space has been surgically defined to its boundaries, the retaining ligaments in the boundary can then be precisely released under direct vision to achieve the desired mobilization while preserving the vital structures closely associated with the ligaments.”
The sub-SMAS facial spaces are “pre-dissected” by nature — they open easily, are bloodless, and contain no facial nerve branches. They provide the surgical highway into the deeper face. The retaining ligaments at their boundaries mark both the sites of maximum laxity (where the correction must occur) and the locations of the facial nerve branches (where the greatest surgical care is required).
Modern facelift surgery exploits this anatomy in three steps:
1. Enter the space via blunt dissection — safe, fast, bloodless
2. Define the boundaries precisely
3. Release the retaining ligaments under direct vision, with the nerve visible and protected
Fixation sutures are placed at the ligament positions — the natural suspension points of the face — rather than at the periphery. “Where fixation sutures are placed in the anterior face in sub-SMAS surgery, they function as replacements for the retaining ligaments that have weakened or have been divided in order to mobilize the composite flap.”
The result is a face that has been structurally restored to a more youthful configuration — not simply pulled tighter at the surface.
Frequently Asked Questions
What is the SMAS and why does it matter for facelift surgery?
The SMAS (Superficial Musculoaponeurotic System) is the continuous fibromuscular sheet of layer 3 that contains the muscles of facial expression and connects the face from scalp to neck. Addressing the SMAS allows the surgeon to reshape the underlying structure of the face — not just tighten the skin surface — producing results that are more natural and more lasting.
Why do jowls form in a specific location?
Jowls form directly behind the mandibular ligament — one of the face’s strongest retaining ligaments — because tissue cannot descend past it. The roof of the premasseter space weakens with age, the platysma descends, and tissue accumulates just behind the fixed mandibular ligament, creating the jowl bulge.
What causes the tear trough?
The tear trough ligament — a true osteocutaneous ligament anchored to the maxilla — tethers the skin at the tear trough position. As the surrounding soft tissue changes with age and the maxilla itself resorbs, this ligament becomes more visible as a groove.
Does fat descend in the ageing face?
Current evidence shows facial fat descends very little. The fat compartments are held in position by the retaining ligaments. What changes with age is that the boundaries between compartments become more visible as the ligaments weaken, and individual compartments may atrophy — creating hollows — while others accumulate descended tissue from adjacent spaces.
Why does the outer brow drop more than the inner brow?
The frontalis muscle — which lifts the brow — ends at the temporal fusion line (superior temporal septum). Lateral to this point, there is no upward-pulling muscle to oppose the brow depressors and gravity, so the outer brow descends preferentially.
How does bone loss contribute to facial ageing?
As the facial skeleton resorbs — particularly the midface, orbital rim, and prejowl mandible — the soft tissue loses its structural foundation. The retaining ligaments anchored to the receding bone pull the skin inward, creating grooves. Meanwhile, the loss of skeletal projection gives a visual impression of soft tissue descent, even when the tissue itself has not moved significantly.
What is the “tired look” caused by?
The characteristic “tired look” of the ageing face is caused by the segmentation of the midcheek into three distinct zones separated by the Y-shaped pattern of the nasojugal, palpebromalar, and midcheek grooves. This segmentation is the surface expression of the underlying spaces and ligament anatomy becoming visible with age.
Are the facial soft tissue spaces dangerous to operate in?
No — by definition, the soft tissue spaces contain no facial nerve branches. They are anatomically safe zones. The facial nerve travels outside and around the spaces. It is at the ligamentous boundaries between spaces — where the nerve transitions from deep to superficial — that surgical care is most critical.
—
Summary
Facial ageing is a multilayered, anatomically governed process. Every visible sign of ageing — the jowl, the tear trough, the midcheek grooves, the hollowed temple, the nasolabial fold — corresponds to a specific change in the underlying five-layer anatomy of the face. The spaces expand. The ligaments weaken. The skeleton resorbs. The skin thins. Each change compounds the others.
Modern facial rejuvenation, at its best, works backwards through this process — restoring structural support where it has been lost, correcting laxity at the anatomical level where it originates, and rebuilding volume where the skeleton and fat have depleted. The result is a face that looks like a younger version of itself — naturally, durably, and without the operated appearance of the past.
Further Reading in This Series
Ross Farhadieh is an internationally recognised plastic and reconstructive surgeon, educator and editor of two landmark reference textbooks in plastic surgery. He works in Canberra and Sydney, He practises at [panthea.com.au](https://www.panthea.com.au).
Text excerpts and diagram descriptions in this article are drawn from chapters authored or edited by Ross Farhadieh in: Plastic Surgery: Practice and Principles, Elsevier, 2021; and Plastic Surgery: Approach and Techniques, Wiley-Blackwell, 2015. All text and illustrations © Ross Farhadieh and respective co-authors. All rights reserved.











