RHINOPLASTY FACTSHEET
THE NOSE
The nose is a complex three-dimensional structure with critical structural and functional roles, which, by virtue of its position, serves as the central component of the face. Its relationship to surrounding structures is in part responsible for a harmonious, pleasing visage as a whole. Functionally, the nose provides an airway and acts to warm, filter and humidify air passing through it. Noses that deviate from ideal structural proportions – whether subtle variations of normal or more dramatic post-traumatic or neoplastic deformities – have motivated rhinoplasty surgeons since ancient India 800 B.C.E.
PATIENT ASSESSMENT
The process of rhinoplasty begins with patient evaluation. Arguably, the foundation of a successful rhinoplasty is established at the initial patient visit, including:
- A thorough, accurate evaluation of the nose;
- Its relation to the rest of the patient’s face;
- Identification of appropriate and realistic goals given the patient’s anatomy;
- Clear communication; and
- Mutual understanding and agreement of surgical goals between the patient and the surgeon.
Meticulous preoperative photo-documentation is compulsory and computer-generate images of potential postoperative goals may be helpful in facilitating patient-surgeon discussion and establishing operative goals.
PHYSICAL EXAMINATION:
Physical exam should include a thorough facial analysis characterising the nasal structures themselves and their relationship to the face as a whole. A careful intranasal exam should also be performed, including inspection of the septum, turbinates, nasal valves and an assessment of nasal breathing. Finger palpation (feeling with the fingers or hands) is an essential component of the exam.
PHOTOGRAPHY:
The standard approach to photography for rhinoplasty is to obtain realistic preoperative photographs. Many surgeons will have a dedicated space for photography in their office. Standardisation of patient positioning, lighting and angles should be maintained. This will facilitate the surgeon’s study of the patient’s nasal anatomy and facial harmony for surgical planning. Moreover, it permits accurate pre- and postoperative comparison.
POSTOPERATIVE CARE
Postoperative care varies among surgeons. Patients are counselled about the potential for postoperative bleeding, which can be self-limited and treated with oxymetazoline spray. In the immediate postoperative period (24-48 hours), patients should keep their head elevated to minimise swelling. Patients should avoid exercise or strenuous activity for 2-4 weeks postoperatively. Sutures and splints are removed one week postoperatively. Although it is not always necessary or indicated, postoperative steroids have been observed to be effective in decreasing swelling.
POTENTIAL COMPLICATIONS
After the rhinoplasty, the normal postoperative course has some expected inconveniences that the patient should be made aware of preoperatively and should not be considered as complications. Pain, bruising and postoperative swelling are to be expected. If the swelling is excessive or prolonged, postoperative oral steroids may help to speed resolution. However, excessive postoperative bleeding is rare (o.9% of cases). Taping the nose may be helpful in decreasing swelling and may be continued by the patient on a nightly basis even weeks after surgery.
In the immediate postoperative period, complications may include:
- Bleeding;
- Erythema (redness of the skin) related to vascular congestion;
- Infection;
- Skin loss or necrosis; and
- Early patient dissatisfaction.
In the intermediate postoperative period (2 weeks – 2 months), complications may include:
- Prolonged swelling;
- Delayed healing;
- Patient concern/dissatisfaction;
- Synechiae (where the iris adheres to either the cornea or lens;
- Osseous overgrowth (consists of/or has turned into bone);
- Septal perforation;
- Anosmia (loss of sense of smell); and
- Late presentation of a cerebrospinal fluid (CSF) leak.
Late complications from rhinoplasty include:
- Nasal airway obstruction;
- Various irregularities and deformities;
- Implant exposure;
- Extrusion or migration;
- Scarring;
- Silent sinus syndrome;
- Enophthalmos (posterior displacement of the eyeball); and
- Mucocele (cyst) formation.
GETTING A RHINOPLASTY WITH DR FARHADIEH
BEFORE RHINOPLASTY SURGERY:
During the initial consultation, Dr Farhadieh will go over your previous medical history by asking for information on the following things:
- High blood pressure
- Blood clotting disorders
- Thyroid disease
- All previous surgeries
- Smoking history
- Allergies and hay fever
- Current medications
Dr Farhadieh will then discuss your aesthetic concerns, as well as any functional issues that may worry you. After examination of your nose and facial features, a set of medical record photographs will be taken and all options will be discussed with you.
Major complications are not common in rhinoplasty and all possible risks will be discussed with you at length during your consultation. Smokers are advised to stop smoking for at least 3–6 weeks both before and after surgery. You will need to stop taking any blood-thinning medications or alternative dietary supplements for at least 2 weeks prior to surgery.
Rhinoplasty is performed either as an outpatient surgery or in the hospital with overnight admission. It’s important to note that you will need someone to drive you home afterwards. Prior to surgery, Dr Farhadieh will mark your nose and face and address any remaining questions with you. The surgery involves internal incisions and often a small external incision (open rhinoplasty), which heals well and is not noticeable. Nose job surgery usually takes between 1 and 2 hours, but can sometimes be longer, especially in cases where it is a revision rhinoplasty or more extensive work is carried out. Depending on the aim, your nose may be built up in areas using your own nasal cartilage, the bridge may be narrowed, the septum straightened and nostrils adjusted if needs be.
AFTER RHINOPLASTY SURGERY:
When you wake up in recovery, there will be a thermoplastic plaster on your nose. You will need to wear this for up to 2 weeks post-surgery. Pain relief will be provided to make you comfortable, as your nose will feel blocked and breathing may seem arduous at first. However, most patients adapt to mouth breathing quickly. If you have been admitted overnight, you will be discharged in the morning after removal of nasal packs.
You will be seen again in our clinic within a week and will have your external sutures removed. The skin of your nose will be partially numb owing to the open technique, but this should recover in time. During the first week to 10 days postoperatively, you should avoid physical activities, especially bending or straining. This decreases likelihood of bleeding and helps reduce swelling. The majority of swelling and any bruising from surgery will settle within the first 3 weeks, and the remainder in the following 3 weeks. Careful management of the skin envelope helps to reduce swelling, especially in those with thick skin. Postoperative photographs will be taken as part of your confidential medical records.
Although you can start walking immediately after discharge, reduced relative activity and no exertion during the first week to 10 days is advised. Social activities can start 10–14 days after surgery, depending on the level of swelling and bruising. Normal sports activities can be recommenced at 6 weeks and contact sports at 3 months.
Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
Gallery
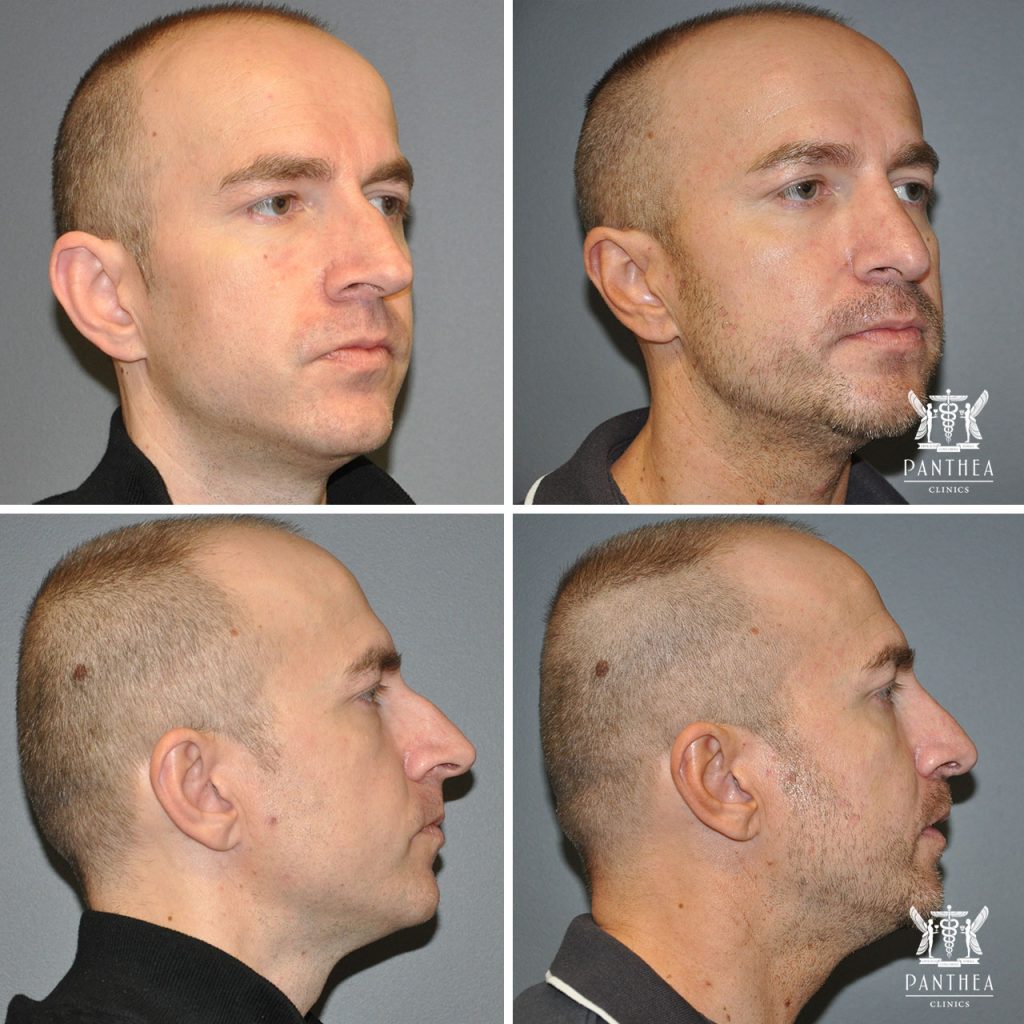
38 Year old Male at 3 month postoperatively who underwent a rhinoplasty procedure.
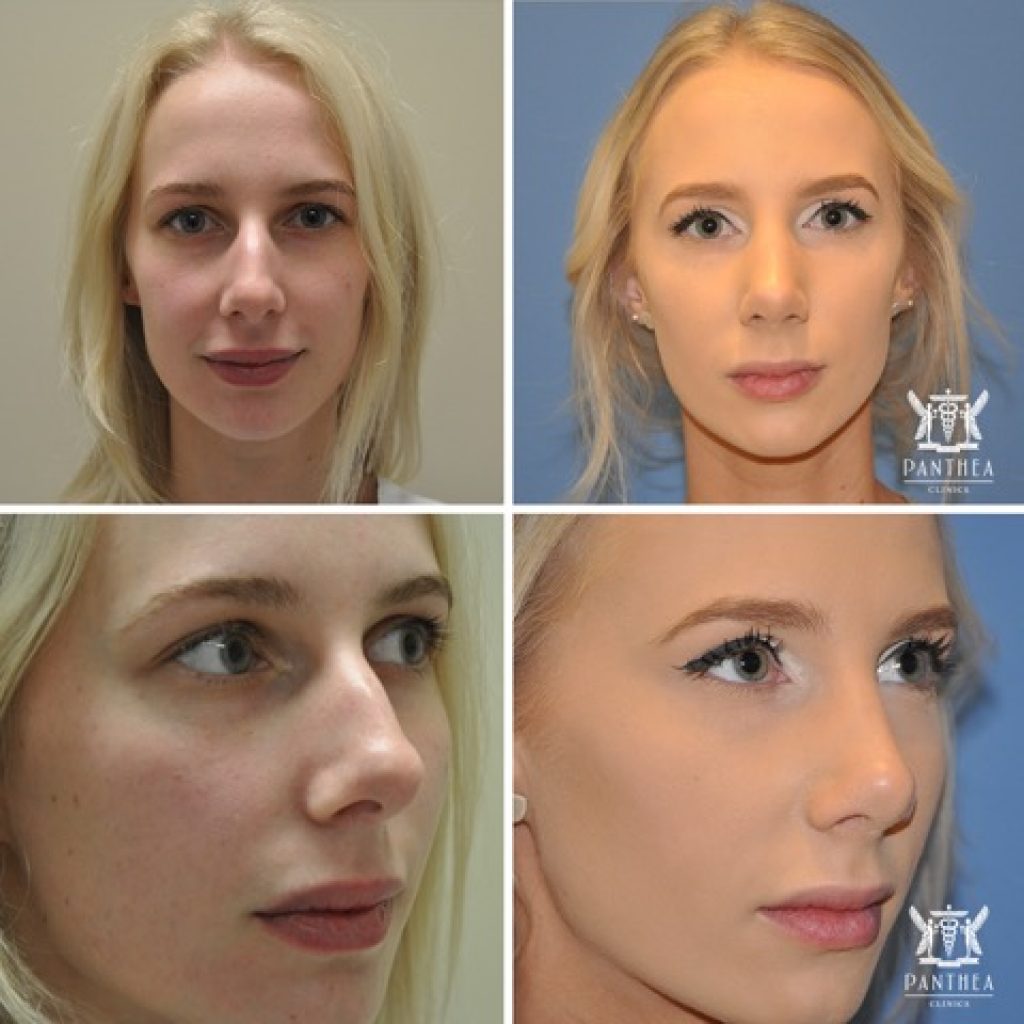
Open rhinoplasty at 6 months in a 20 year old.
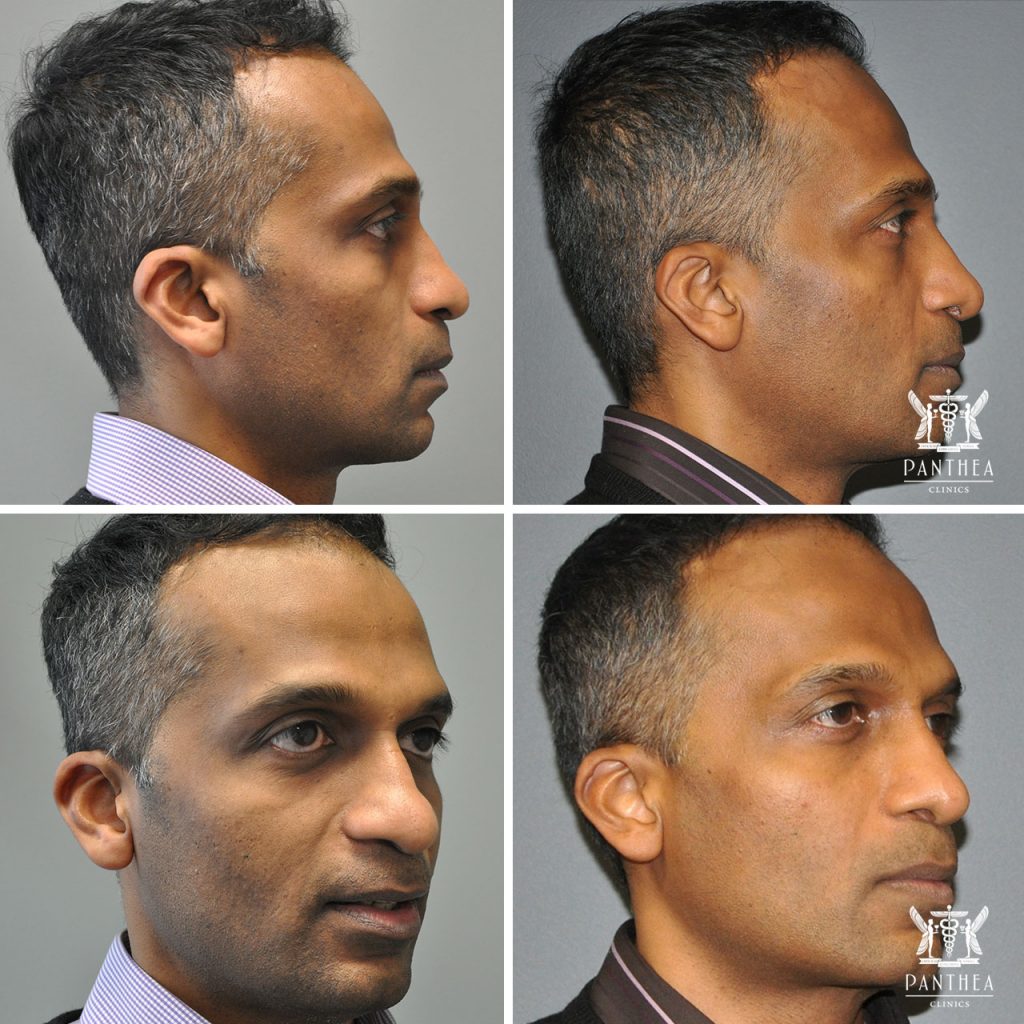
Revision rhinoplasty with rib reconstruction of nasal support after primary rhinoplasty elsewhere at 4 months postoperatively in a 42 year old man.
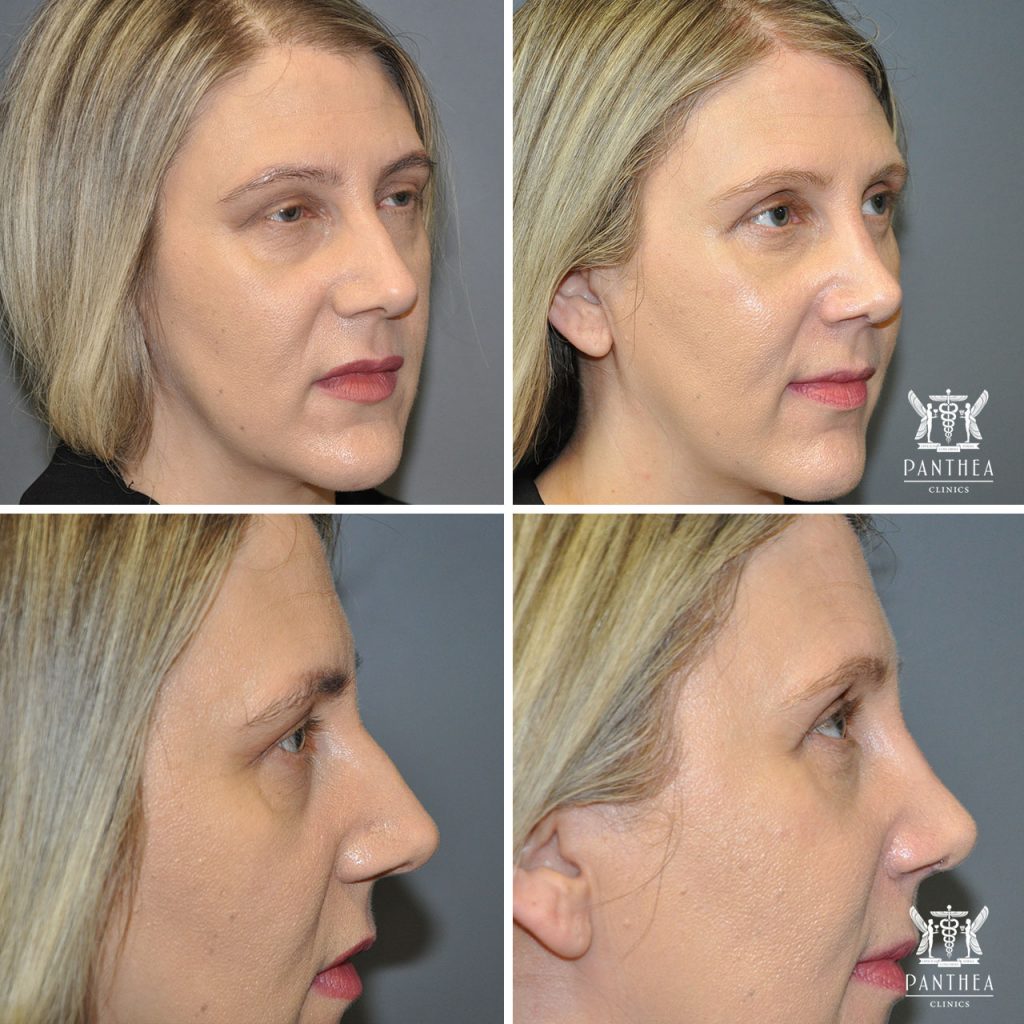
43 year old women who underwent a rhinoplasty at 3 moths postoperatively.










